Integrating Oral Health into Community Health Equity Initiatives

Community health equity initiatives tend to address chronic disease, mental health, and access to primary care. Yet oral health rarely makes it into the conversation. This separation persists even though oral health disparities follow the same fault lines as broader health inequities, disproportionately affecting low-income communities, communities of color, and rural populations.
Closing this gap calls for more than added programming. It demands structural changes to how oral health equity is framed, funded, and integrated into existing public health infrastructure.
Why Oral Health Disparities Persist
Children living in high-poverty households are more than twice as likely to have untreated dental decay compared to their higher-income peers, according to CDC data on oral health disparities. These gaps are not isolated to income alone. They cut across race and ethnicity, education level, and geography, reflecting the deeper influence of social determinants of health on who receives care and who goes without.
Medicaid coverage for dental services varies widely from state to state, leaving millions in what amount to access deserts. Where coverage does exist, low reimbursement rates discourage providers from accepting Medicaid patients, shrinking the pool of available care even further.
Rural communities face these barriers in compounding layers. Fewer dental providers, longer travel distances, and limited insurance acceptance create conditions where routine preventive care becomes difficult to access. Community dental practices such as RivertownDentalOnline.com and other local providers serve as critical access points in these underserved areas, helping bridge the distance between residents and reducing oral health inequalities at the ground level.
Still, individual practices and programs cannot close these oral health disparities on their own. Without systemic support through policy, funding, and workforce investment, the structural causes behind these inequities will continue to persist.
Policy Levers That Drive Integration
Several policy mechanisms can move oral health integration from aspiration to standard practice. At the state level, expanding adult Medicaid dental benefits remains one of the most direct paths to closing coverage gaps. States that have added comprehensive adult dental benefits under Medicaid have seen measurable increases in utilization, particularly among populations that previously went without care entirely.
Reimbursement rates matter just as much as coverage itself. When Medicaid dental reimbursement falls well below market rates, providers opt out, and coverage on paper fails to translate into actual appointments. Raising these rates draws more providers into the network and shortens wait times for patients who need care most.
Beyond coverage, primary care integration offers a practical way to reach patients who may never visit a dentist. Embedding dental screenings and fluoride varnish applications into well-child visits and chronic disease management appointments brings oral health equity efforts into settings patients already trust and use. This model of oral health integration has gained traction in states like Colorado and Oregon, where policy mandates now support interprofessional collaboration between medical and dental teams.
These approaches reflect a broader shift toward treating preventive dentistry in reducing health disparities as a public health priority rather than an afterthought.
Workforce and Delivery Models Closing the Gap
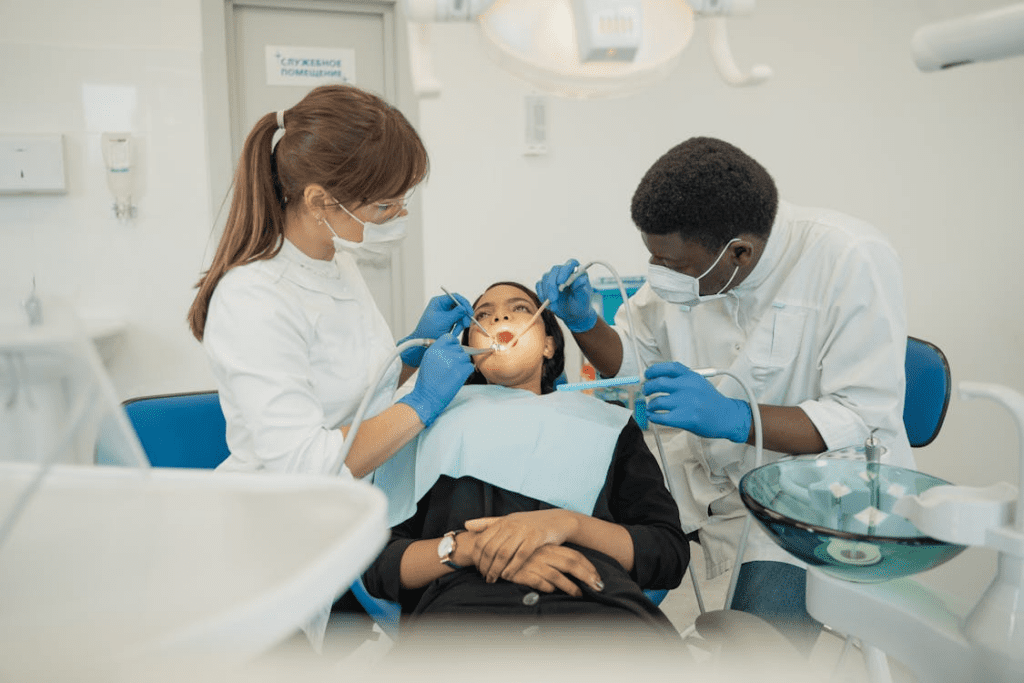
Policy changes create the foundation, but delivery depends on having the right people in the right places. Across much of the country, the dental workforce is unevenly distributed, with rural communities and low-income urban neighborhoods facing persistent provider shortages that no single policy fix can resolve.
Dental therapists have emerged as one of the more effective responses to this gap. Functioning as mid-level providers, they perform preventive and restorative procedures under the supervision of a dentist, extending the reach of practices that would otherwise turn patients away. States like Minnesota and Maine have authorized dental therapists specifically to address access barriers in underserved areas.
Community health workers fill a different but equally important role. They connect residents to oral health resources, help families navigate insurance enrollment, and deliver culturally appropriate education about prevention. Their value lies in proximity and trust, two things that clinical systems alone often struggle to build.
School-Based Programs and Teledentistry
School-based dental programs bring care directly to children who might otherwise miss it entirely. Sealant programs, screenings, and fluoride treatments delivered on school grounds eliminate transportation and scheduling barriers that keep low-income families from accessing preventive care.
Teledentistry adds another layer of flexibility. In remote areas where a dental office may be an hour or more away, virtual consultations allow providers to triage urgent cases, guide follow-up care, and conduct preliminary assessments without requiring an in-person visit. While it does not replace hands-on treatment, it keeps patients connected to providers between appointments.
No single model addresses every barrier on its own. The most effective community-level strategies layer these approaches together, pairing workforce expansion with school-based dental programs, teledentistry, and community health workers to cover gaps that each model leaves individually.
What Meaningful Integration Looks Like
Oral health cannot remain a separate lane in health equity work. The strategies outlined across policy reform, workforce development, and community delivery models are most effective when they operate as a coordinated system rather than isolated initiatives. Communities that layer multiple approaches together, expanding coverage while also investing in dental therapists, school-based programs, and culturally grounded outreach, tend to see the strongest outcomes. True oral health integration requires each of these pieces to reinforce the others.