Benefits of Minimally Invasive Spine Surgery for Chronic Pain
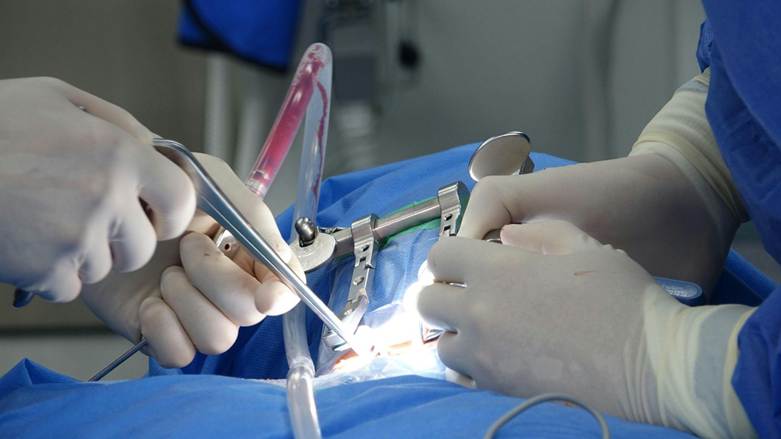
If you’re dealing with chronic pain, you might find relief through Minimally Invasive Spine Surgery (MISS). This advanced technique reduces muscle and tissue trauma compared to traditional methods. With its precision, MISS targets pain’s root causes, offering long-term relief. Patients often experience shorter recovery times and improved mobility. Plus, there’s a lower risk of complications, making it a cost-effective option. Curious about how MISS could transform your pain management?
Understanding Minimally Invasive Spine Surgery
Minimally invasive spine surgery (MISS) represents a significant advancement in surgical techniques, offering numerous benefits over traditional open surgery. With MISS, you can expect reduced trauma to surrounding tissues, leading to a quicker recovery and less postoperative pain. Central to its success are modern techniques for minimally invasive spinal procedures that combine advanced surgical planning and enhanced imaging technologies, allowing for precise targeting of affected areas. These methods facilitate smaller incisions and improved visualization, essential for effective intervention.
Advanced surgical planning involves detailed preoperative evaluation using state-of-the-art imaging methods like MRI or CT scans. Enhanced imaging techniques, such as intraoperative navigation systems, provide real-time feedback, ensuring ideal alignment and placement of surgical instruments. By minimizing disruption to healthy tissues, MISS enhances outcomes, making it a preferred option for treating chronic spinal conditions.
Comparing Traditional and Minimally Invasive Techniques
While understanding the benefits of minimally invasive spine surgery is essential, it’s equally important to examine how these techniques stack up against traditional open surgery. In surgical approach evaluation, minimally invasive methods utilize smaller incisions and specialized instruments, reducing hospital stays and accelerating recovery. Conversely, traditional surgery involves larger incisions, potentially leading to longer rehabilitation. Critical to both methods is patient selection criteria. Not every case is suitable for minimally invasive procedures; factors like spinal anatomy and the specific condition dictate the ideal approach. Evidence suggests that when appropriately selected, patients undergoing minimally invasive surgery experience less postoperative pain and quicker return to daily activities. However, traditional surgery might be necessary for more complex cases, underscoring the need for expert evaluation in treatment planning.
Reduced Muscle and Tissue Trauma
Imagine undergoing spine surgery and discovering that your recovery involves minimal discomfort and rapid healing. Minimally invasive spine surgery offers this advantage due to its smaller incision size, which drastically reduces muscle and tissue trauma. By employing advanced techniques, surgeons can navigate through your body with precision, ensuring less tissue disruption. This approach preserves the integrity of surrounding muscle structures, leading to reduced postoperative pain and inflammation. Evidence supports that patients experience fewer complications and improved functional outcomes compared to traditional methods. The focused nature of the procedure minimizes collateral damage to muscles and ligaments, enhancing overall recovery. Fundamentally, the minimally invasive approach prioritizes your comfort and accelerates healing by minimizing trauma to critical anatomical structures.
Shorter Recovery Time
When recovering from spine surgery, you’ll find that minimally invasive techniques markedly shorten your recovery time due to their precision and reduced impact on the body. These advanced methods employ smaller incisions, resulting in less disruption to surrounding tissues, thereby promoting an improved rehabilitation process. By minimizing trauma, these procedures support a considerably faster return to daily activities, a key advantage over traditional open surgery. Clinical studies have demonstrated that patients undergoing minimally invasive spine surgery experience reduced hospital stays and quicker overall recovery periods. Enhanced surgical precision and targeted intervention allow for less postoperative discomfort, enabling you to engage in physical therapy sooner. As a result, you’ll regain mobility and independence faster, making minimally invasive techniques a superior choice for chronic pain management.
Lower Risk of Postoperative Complications
Minimally invasive spine surgery (MISS) considerably reduces the risk of postoperative complications, a major benefit that distinguishes it from traditional open surgery methods. By utilizing smaller incisions and advanced imaging techniques, MISS limits tissue disruption and blood loss. This precision leads to fewer complications such as infections and hemorrhages. As a result, patients experience a decreased hospital stay, often returning home sooner compared to those undergoing open surgery. Additionally, the reduced postoperative pain associated with MISS minimizes the need for strong analgesics, thereby lowering the risk of medication-related side effects. The streamlined recovery process and reduced complication rates make MISS a preferred option for managing chronic pain, providing a safer, more efficient surgical experience.
Enhanced Precision and Accuracy
Due to advancements in technology and surgical techniques, minimally invasive spine surgery (MISS) offers heightened precision and accuracy, pivotal elements in treating chronic pain effectively. With enhanced surgical visualization, surgeons can now see intricate anatomical structures like never before, reducing the risk of damaging surrounding tissues. Optimized surgical access allows for smaller incisions, decreasing the odds of infection and scarring.
Key benefits of heightened precision and accuracy in MISS include:
- Targeted Intervention: Surgeons can precisely address the pain source, improving outcomes.
- Reduced Tissue Trauma: By focusing only on affected areas, collateral tissue damage is minimized.
- Shorter Recovery Time: Precision guarantees faster healing, aiding in a quicker return to daily activities.
These advancements contribute considerably to the efficacy of MISS in managing chronic pain.
Improved Patient Mobility
Although traditional spine surgery can be effective, minimally invasive spine surgery (MISS) considerably enhances patient mobility post-operation. By reducing tissue disruption, MISS facilitates quicker recovery, promoting increased flexibility and an enhanced range of motion. The smaller incisions used in MISS minimize muscle damage, preserving the structural integrity necessary for paramount movement. Studies indicate that patients undergoing MISS exhibit improved functional outcomes, as the procedure supports the restoration of natural spinal alignment. This alignment is indispensable for balanced weight distribution across the spine, further contributing to mobility improvements. Additionally, less postoperative pain and reduced scarring allow you to engage in rehabilitation exercises sooner, accelerating the return to daily activities. Consequently, MISS provides a more effective pathway to regaining mobility and overall physical function.
Long-Term Pain Relief
In many cases, minimally invasive spine surgery (MISS) delivers long-term pain relief by targeting the underlying causes of chronic discomfort with precision. This approach offers significant advantages for long term symptom management and lasting pain resolution. By addressing the root of your pain with less tissue disruption, MISS facilitates sustained recovery and decreased reliance on analgesics.
- Precision Targeting: MISS techniques allow for precise intervention, minimizing damage to surrounding tissues.
- Reduced Recovery Time: With smaller incisions, you’ll likely experience a quicker return to daily activities.
- Enhanced Outcomes: Studies have shown that patients often report significant long-term symptom management, improving quality of life.
Incorporating these advanced surgical techniques can lead to meaningful and enduring relief, empowering you to reclaim a pain-free existence.
Cost-Effectiveness of MISS
While the long-term pain relief provided by minimally invasive spine surgery is a compelling reason for its consideration, understanding its cost-effectiveness is equally important. A rigorous cost effectiveness analysis reveals that MISS offers significant economic benefits by reducing hospital stays and rehabilitation times. Shorter recovery periods translate to less time off work, which can result in substantial savings for patients and insurers alike. Additionally, the precision of MISS often leads to fewer complications, minimizing the need for costly follow-up procedures. Studies indicate that although initial costs may be higher compared to traditional surgery, the overall reduction in healthcare expenditure makes it a financially viable option. Consequently, MISS stands as a cost-effective solution in addressing chronic spine-related pain.
Access to MISS: What Patients Need to Know
If you’re considering minimally invasive spine surgery (MISS) for chronic pain, understanding access to this advanced treatment is indispensable. Determining whether MISS is right for you involves a structured approach. Key aspects to focus on include:
- Patient Eligibility Criteria: Not everyone qualifies for MISS. Factors like age, general health, and specific spinal condition are assessed to guarantee ideal outcomes.
- Preoperative Evaluation Process: This essential step involves exhaustive diagnostic imaging and medical history analysis to tailor the surgical approach to your unique needs.
- Consultation with Specialists: Engaging with a multidisciplinary team ensures that all aspects of your health are considered, optimizing both safety and efficacy.
Frequently Asked Questions
How Does Minimally Invasive Spine Surgery Affect Lifestyle Changes Post-Surgery?
Minimally invasive spine surgery can substantially enhance your lifestyle post-surgery. You’ll experience reduced recovery time, allowing quicker return to daily activities, and improved mobility, enabling better physical function. These changes are supported by evidence-based outcomes and clinical expertise.
Are There Specific Exercises Recommended After Minimally Invasive Spine Surgery?
Yes, post-surgery physical therapy often includes specific exercises like gentle stretches and core strengthening. You’ll gradually return to activity, focusing on improving flexibility and stability, while evidence-based protocols guarantee a safe recovery process.
What Anesthesia Is Typically Used During Minimally Invasive Spine Surgery?
You’ll typically encounter general anesthesia for minimally invasive spine surgery, guaranteeing you’re unconscious. Anesthesia options may also include regional anesthesia. Intraoperative monitoring techniques, like neurophysiological monitoring, help safeguard safety by tracking nerve function throughout the procedure.
How Do Patient Eligibility Criteria Differ for Minimally Invasive Spine Surgery?
You’ll find patient eligibility for minimally invasive spine surgery varies, focusing on thorough assessment of your medical history and precise imaging test results. Surgeons evaluate these details to guarantee you’re a suitable candidate, minimizing risks and optimizing outcomes.
Can Minimally Invasive Spine Surgery Be Performed on All Spinal Conditions?
Minimally invasive spine surgery isn’t suitable for all spinal conditions. It’s typically applicable to limited spinal conditions due to certain surgical techniques. Evidence shows it’s effective for specific issues like herniated discs and spinal stenosis, not all-encompassing degenerative diseases.